
Office Hours
By Appointment Only
At the office of Brittney K. Craig, DMD, our first goal is to preserve natural teeth whenever it is safe and sensible to do so. Still, there are times when removing a tooth becomes the healthiest option for the mouth as a whole. A careful evaluation helps us weigh the risks and benefits so that any extraction we recommend supports your overall oral function and future treatment planning.
Extractions are never a one-size-fits-all decision. We consider the tooth’s condition, its role in chewing and speech, the health of surrounding teeth and bone, and the patient’s medical history. Removing a problematic tooth can relieve pain, stop the spread of infection, prevent damage to adjacent teeth, and prepare the mouth for restorative treatment when necessary.
Below are some of the most common clinical reasons an extraction may be advised. Each item reflects a distinct situation and may lead to a different type of removal or follow-up plan.
Primary (baby) teeth that won’t shed naturally
Sometimes a primary tooth remains firmly attached past the expected time for exfoliation. This can be due to retained roots, ankylosis (fusion to the bone), or developmental variance. If an over-retained baby tooth prevents the normal eruption of its permanent successor, a gentle extraction may be the best path to prevent misalignment and other complications.
Permanent teeth that are too damaged to restore
When decay or trauma has destroyed most of a tooth’s structure or the root is irreparably infected, restoring the tooth may not be possible or predictable. In those cases, removing the tooth can eliminate infection, protect nearby teeth, and allow for future replacement options that restore comfort and function.
Teeth with severe fractures extending below the gumline
A complex fracture that compromises the root or leaves insufficient tooth structure above the gum can make restoration unfeasible. Extraction prevents chronic pain and recurrent infection when a fractured tooth cannot be reliably rebuilt.
Advanced periodontal disease affecting tooth support
Periodontal disease damages the tissues and bone that hold teeth in place. When support becomes hopeless and teeth are mobile or painful, extraction can help control disease progression and simplify subsequent periodontal or restorative care.
Wisdom teeth that are impacted, poorly positioned, or decayed
Third molars often run out of space or erupt at awkward angles, which can lead to decay, infection, or damage to neighboring teeth. Removing problematic wisdom teeth, especially when they threaten adjacent structures, is a common preventive or corrective step.
Extractions as part of orthodontic treatment
When the jaw cannot comfortably accommodate all permanent teeth, removing select teeth can create the space needed to achieve a balanced, functional bite. Extractions in orthodontics are carefully planned with long-term alignment and facial proportions in mind.
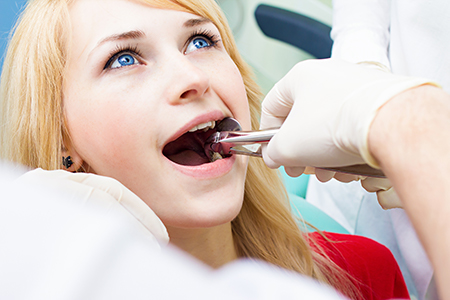
Before any extraction, we perform a thorough review of your medical and dental history so that the procedure is tailored to your specific needs. This includes a discussion of current medications, medical conditions, and any allergies. In some circumstances, we coordinate with your physician or request medical clearance to ensure the safest approach.
Diagnostic imaging—such as digital radiographs—lets us assess root shape, bone density, tooth position, and proximity to vital structures. Those images guide whether a tooth can be removed simply or if a more involved surgical approach will be required. We’ll explain the findings and what they mean for your treatment so you can make an informed choice.
Your comfort is a priority. Local anesthesia is standard for extractions, and we will review sedation options for patients who experience significant anxiety or for procedures that are more complex. We’ll also provide clear pre-operative instructions and answer any questions you have ahead of the appointment.
A simple extraction generally applies to teeth that are visible in the mouth and have uncomplicated root anatomy. After numbing the area, the dentist gently loosens the tooth and removes it with forceps. The goal is to complete the removal with minimal trauma to the surrounding tissues and a smooth recovery.
Surgical extractions are used for teeth that are broken at the gumline, impacted, or have complex root structures. The procedure may require a small incision, careful removal of a bit of bone, and sectioning the tooth for safer extraction. In some cases, we may refer to an oral and maxillofacial surgeon when the surgical complexity calls for specialized expertise.
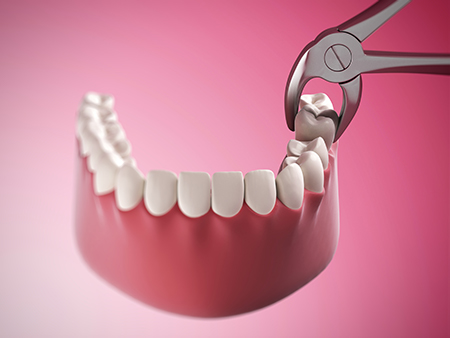
Following an extraction, a focused recovery plan helps manage discomfort and reduce the risk of complications. We provide personalized post-op instructions that cover pain control, activity restrictions, and oral hygiene tailored to the type of extraction performed. Adhering to these directions supports clot stability and encourages predictable healing.
Most patients can manage mild discomfort with over-the-counter or prescription medications taken as directed. We also provide guidance on swelling control, dietary choices, and habits to avoid that can interfere with healing. If sutures are placed or if there are additional concerns, a follow-up visit is scheduled to monitor healing and remove stitches if needed.
Contact our office if you experience heavy bleeding, increasing pain, fever, or any unusual symptoms. Early communication allows us to intervene promptly if a problem arises.
Maintain gentle pressure with gauze
Bite on the provided gauze pad as instructed to help the socket clot. Replace the gauze after the initial hour if necessary and continue to follow any timing directions your clinician gives you.
Protect numb tissues
Avoid chewing, touching, or putting hot foods where the area is numb to prevent accidental biting of the lip, cheek, or tongue until sensation returns.
Take medications as directed
If antibiotics are prescribed, complete the full course. For pain control, take anti-inflammatory or prescription medications according to instructions and timing to minimize discomfort.
Preserve the clot
Do not rinse vigorously, spit forcefully, or use a straw for the first 24–48 hours. These actions can dislodge the clot and delay healing.
Manage swelling
Apply an ice pack to the outside of the face in short intervals during the first day to keep swelling and discomfort in check.
Avoid tobacco use
Smoking and vaping hinder clot formation and slow healing. Refrain from tobacco products for at least a week following the extraction when possible.
Choose soft, nourishing foods
Stick with lukewarm or cool soft items for the first few days and stay hydrated. Avoid hot, spicy, or carbonated beverages until the area has stabilized.
Keep oral hygiene gentle
Brush carefully around the surgical area, and once appropriate, rinse with a mild saltwater solution to keep the socket clean without disturbing the clot.
Attend scheduled follow-up
Return for any post-operative checks so we can confirm healing is progressing and address questions about replacement options when appropriate.
Each life stage presents different extraction considerations. With children, timing matters: removing a retained baby tooth at the right time can encourage proper eruption patterns. For adolescents and young adults, wisdom teeth are evaluated for space, angulation, and potential to cause future problems.
Impacted or partially erupted third molars can trap food and bacteria, leading to decay or recurrent infections. When a wisdom tooth threatens neighboring teeth or causes chronic symptoms, removal can prevent more serious issues. Conversely, if a wisdom tooth is healthy, fully erupted, and easy to clean, we may recommend monitoring rather than immediate extraction.
Orthodontic plans sometimes require extractions to create room for proper alignment. These decisions are made in close collaboration with your orthodontist to achieve stable, aesthetically pleasing, and functional results. We coordinate with other specialists as needed so your treatment flows smoothly from extraction to the next phase of care.
We combine careful clinical judgment with gentle technique to make extractions as comfortable and predictable as possible. Our team prioritizes clear communication: you’ll understand why a removal is recommended, what to expect during the procedure, and how to care for yourself afterward.
If a missing tooth will need replacement, we’ll discuss appropriate options — from removable dentures to fixed bridges to dental implants — and the sequence of care that best meets your goals. Our focus is on long-term oral health, function, and a natural appearance.
We strive to make each visit calm, respectful, and tailored to your needs. If you have questions about extractions or want to explore alternatives and follow-up care, please contact us for more information.
A tooth extraction is recommended when retaining the tooth would harm overall oral health or when restoration is no longer predictable. Common clinical reasons include severe decay with little remaining structure, unrestorable fractures that extend below the gumline, irreversible root infections, and advanced periodontal disease that leaves the tooth without adequate support. Wisdom teeth that are impacted, recurrently infected, or damaging neighboring teeth are also frequent reasons for removal.
Decisions about extraction are individualized and consider the tooth's role in chewing and speech, the condition of surrounding teeth and bone, and the patient's medical history. We weigh alternatives—such as root canal therapy, crown restoration, or periodontal treatment—against the risks and benefits of removal to select the option that best preserves long-term function. When extraction is advised, the goal is to relieve symptoms, control infection, and plan for appropriate follow-up care or replacement if needed.
The choice between a simple and a surgical extraction depends on how accessible the tooth is and the complexity of its root anatomy. Simple extractions typically apply to teeth that are fully erupted and have uncomplicated root shapes; these are removed with forceps after effective local anesthesia. Surgical extractions are used for broken teeth, impacted teeth, or teeth with multiple or curved roots and may require a small incision, removal of a bit of bone, or sectioning of the tooth for safe removal.
Diagnostic imaging such as digital radiographs helps assess root form, proximity to vital structures, and bone density to guide this decision. Your clinician will explain the planned technique, why it is recommended, and whether a referral to an oral surgeon is appropriate for more complex cases. Clear preoperative planning reduces surprises and supports a predictable outcome.
On the day of the extraction you will receive a review of your medical and dental history and an explanation of the procedure so you know what to expect. Local anesthesia is typically used to numb the area, and sedation options may be discussed for patients with significant anxiety or for more complex procedures. The clinician will then proceed with the planned technique—simple or surgical—while taking steps to minimize tissue trauma and maintain a sterile field.
After the tooth is removed, the socket may be gently cleansed and, if indicated, sutures placed to support healing. You will receive concise post-operative instructions covering bleeding control, medications, diet, and oral hygiene, and a follow-up appointment may be scheduled to monitor healing. If any unexpected symptoms occur after you go home, the office should be contacted promptly for advice and early intervention.
Preparation begins with a thorough health history and a review of current medications, including blood thinners, antibiotics, and any medical conditions that may affect healing. In some cases your dentist may request medical clearance from your physician or recommend timing the procedure around other treatments to ensure safety. Follow any preoperative directions you are given, such as fasting instructions for sedation and guidance about continuing or pausing specific medications per your provider's advice.
Arrange for transportation if you will receive sedation and plan to rest for the remainder of the day following the procedure. Prepare soft, cool or lukewarm foods and have basic supplies on hand, such as gauze, an ice pack, and any prescribed medications. Clear communication with your dental team about anxiety, prior complications, or special needs helps the visit go smoothly and safely.
Extractions are routine but not without risks; common concerns include bleeding, infection, swelling, and delayed healing. One specific complication is dry socket, where the blood clot that normally protects the socket is dislodged; this condition causes increased pain and is managed with local dressings and targeted pain control. The dental team reduces risks by using sterile technique, providing clear post-operative instructions, and prescribing antibiotics when clinically appropriate.
Patients should follow directions to preserve the clot, avoid smoking, and maintain gentle oral hygiene to reduce complications. If heavy bleeding, fever, worsening pain, or other unusual symptoms develop, prompt contact with the practice allows for timely assessment and treatment. Most complications can be managed successfully when they are identified early and treated appropriately.
Effective post-operative care supports clot formation and reduces discomfort. Bite on gauze as instructed to control bleeding, apply ice to limit swelling during the first 24 hours, and rest with your head elevated; avoid spitting, rinsing vigorously, or using a straw for the first 24–48 hours to protect the clot. Take medications exactly as prescribed and complete any antibiotic course if one was provided.
After the initial period you can gently clean the surrounding teeth and, when advised, begin gentle saltwater rinses to keep the socket clean. Stick with soft, nourishing foods and avoid tobacco to promote faster healing. Attend any scheduled follow-up so the clinician can confirm progress and remove sutures if necessary.
Initial soft tissue healing usually occurs within one to two weeks, while complete bone remodeling of the extraction site can take several months. Many patients are able to resume light, nonstrenuous activities within 24–48 hours, but you should avoid heavy lifting, vigorous exercise, and activities that increase blood pressure during the early healing period to minimize bleeding and swelling. Pain and swelling typically peak in the first 48–72 hours and then gradually improve.
Your dentist will give specific guidance about when you can return to normal oral hygiene routines and other activities based on the complexity of the extraction and your individual healing. If sutures were placed, a follow-up visit will confirm that healing is progressing and determine whether stitch removal is needed. Report any prolonged or worsening symptoms so they can be evaluated without delay.
Follow-up appointments are often scheduled to check healing, remove sutures if present, and discuss next steps for tooth replacement when appropriate. If the extracted tooth affects chewing, speech, or esthetics, your team will review restorative options—such as removable prosthetics, fixed bridges, or dental implants—and explain the recommended sequence of care. Timing for replacement depends on factors like bone volume, the need for grafting, and overall treatment goals.
When long-term replacement is planned, preserving bone and soft tissue may be addressed at the time of extraction with grafting or temporary solutions to support future outcomes. The clinician will present a clear treatment plan, coordinate care with specialists as needed, and explain what to expect during each phase of restorative treatment. Regular checkups ensure the replacement proceeds on schedule and that oral health is maintained.
Extractions in children are common and are approached with special attention to growth and development. Primary (baby) teeth are removed when they fail to exfoliate naturally, block eruption of permanent teeth, or are hopelessly decayed or infected. Timing is important: removing an over-retained primary tooth at the appropriate time can prevent impaction or misalignment of the permanent successor.
When treating pediatric patients, clinicians consider behavioral management, appropriate anesthesia or sedation, and coordination with parents to reduce anxiety and ensure cooperation. After extraction, follow-up monitoring helps confirm normal eruption patterns and identify whether orthodontic consultation or space-maintaining measures are needed to guide development.
Our practice combines careful clinical judgment with techniques designed to make extractions as comfortable and predictable as possible. We prioritize clear communication so you understand why a removal is recommended, the steps of the procedure, and the post-operative care needed to support healing and minimize complications. Diagnostic imaging, comprehensive medical review, and attention to patient comfort guide every treatment plan.
When replacement of a missing tooth is anticipated, we discuss appropriate options and the sequence of care that best meets your functional and esthetic goals, coordinating with specialists as necessary. Our team strives to create a calm, respectful environment where patients feel informed and supported from consultation through recovery and any subsequent restorative care.