
Office Hours
By Appointment Only
Tooth loss affects more people than many expect, but replacing missing teeth is no longer limited to removable options. Dental implants use biocompatible posts to recreate the foundation of a tooth so restorations can look, feel, and function much like the natural tooth they replace. When planned and placed correctly, implants can rebuild chewing ability, improve speech, and restore facial support in a way that preserves long-term oral health.
At Brittney K. Craig, DMD, our approach begins with a careful evaluation of each patient’s needs and goals. We combine clinical examination, dental imaging, and a clear conversation about expectations so every treatment plan reflects both medical considerations and the smile a patient wants to achieve. This emphasis on individualized planning is what helps implants deliver consistently reliable results.
Implant dentistry isn’t simply about filling a gap — it’s about restoring a balanced bite and protecting the surrounding teeth and bone. By replacing missing tooth roots, implants help preserve bone volume and maintain facial contours, reducing the long-term changes that often follow untreated tooth loss.

An implant consists of a surgically placed post that eventually integrates with the jawbone, plus a carefully designed restoration that recreates the visible portion of the tooth. This two-part system provides stability and chewing force much closer to that of a natural tooth than traditional removable options. Because the implant is anchored in bone, it transmits normal chewing forces in a way that helps maintain bone health rather than allowing bone to resorb.
This stability translates to practical benefits: you can eat a wider variety of foods with confidence, speak clearly without worrying about shifting prostheses, and enjoy a predictable long-term outcome when implants are matched with high-quality crowns, bridges, or dentures. The restorative component is designed to blend with the color, shape, and texture of your existing teeth for a natural appearance.
With careful maintenance and routine professional care, dental implants offer durable solutions for single-tooth replacements as well as comprehensive rehabilitations. Their longevity depends on factors like placement precision, oral hygiene, and ongoing dental visits — all elements we emphasize during planning and follow-up care.
Your first implant visit focuses on gathering information and setting a clear treatment roadmap. Digital X-rays and intraoral imaging allow us to assess bone volume, tooth relationships, and any restorative requirements. We’ll review your medical and dental history, answer questions about the procedure, and outline the recommended sequence of care so you know what to expect from start to finish.
Because every mouth is different, the conversation often includes options for restorations, the number and location of implants needed, and whether preparatory procedures such as extractions or bone grafting are advisable. We present this information in straightforward terms so patients can make informed decisions without feeling overwhelmed by technical detail.
Preparing for surgery and recovery is part of our planning process. We’ll discuss anesthesia or sedation options and provide practical pre-op and post-op instructions to help you manage comfort during healing. Clear communication before the procedure helps ease anxiety and supports smoother recoveries.
When just one tooth is missing, an implant plus a crown can restore that tooth without changing the adjacent natural teeth. Unlike a traditional three-unit bridge, a single implant stands on its own and avoids grinding down healthy neighboring teeth. This approach preserves more natural tooth structure while returning full function and a lifelike appearance.
The crown that attaches to the implant is custom-crafted to match your bite and tooth shade, and it can be made from durable ceramic materials for a result that blends seamlessly with surrounding teeth. For many patients, single-tooth implants are the most conservative long-term solution.
When several teeth are missing in a row, an implant-supported bridge can replace them without relying on adjacent natural teeth for support. Strategically placed implants act as supports for multiple connected crowns, which maintains bone stimulation in the area and reduces the need to alter healthy teeth for traditional bridgework.
This option is especially useful when several neighboring teeth are missing or when long-term preservation of the oral structures is a priority. The end result restores chewing function and helps maintain the shape of the jaw and lower face.
For patients missing an entire upper or lower arch, modern implant protocols can provide a permanent-feeling set of teeth using as few as four to six implants. These full-arch restorations can be designed as non-removable (fixed) bridges or as more accessible hybrid dentures that snap onto implants for improved retention. Either approach avoids many limitations of traditional dentures.
These comprehensive restorations are planned with temporary teeth placed immediately in some cases, followed by a final prosthesis once healing and integration are complete. The goal is to restore a functional, natural-looking smile that is stable for eating and speaking.
Implant-retained (or overdenture) designs attach to a small number of implants and offer a significant upgrade in retention and comfort compared with conventional dentures. These dentures clip or snap onto implant abutments, which minimizes movement, improves chewing efficiency, and removes the need for adhesives in many cases.
Because they’re removable for cleaning, implant-retained dentures can combine the hygiene advantages of removable prosthetics with the stability benefits of implant support — a good middle-ground solution for many patients.
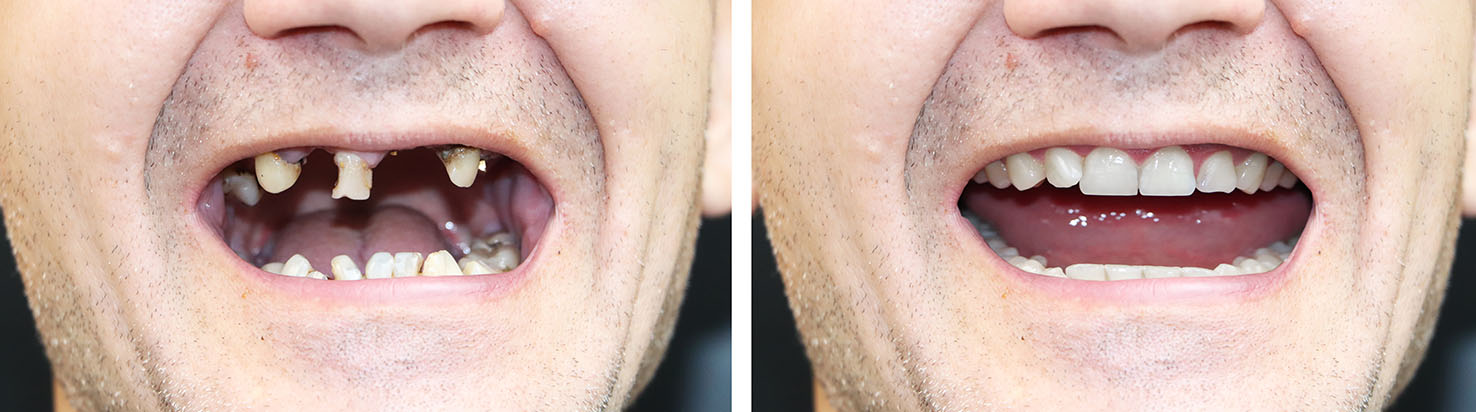
Most adults who are free of uncontrolled medical conditions and who have sufficient bone volume are candidates for dental implants. During an evaluation we consider overall health, medications, gum health, and the expected ability to maintain good oral hygiene. Factors such as smoking or certain systemic conditions can influence planning, but many concerns can be managed so patients still achieve successful outcomes.
Rather than relying on a single benchmark, candidacy is established through a combination of clinical assessment and imaging. This allows us to recommend the treatment path that balances predictability, function, and aesthetics for each patient’s unique situation.
When implants are part of a broader treatment plan, we coordinate any necessary preliminary care — such as periodontal therapy or extractions — to ensure the mouth is healthy and ready for predictable implant integration.
Long-standing tooth loss and certain dental conditions can reduce the available bone at an implant site. In those cases, grafting procedures rebuild the foundation so an implant will have adequate support. Bone grafting uses materials designed to encourage new bone growth and can be performed at the time of extraction or as a separate preparatory step prior to implant placement.
Sinus augmentation is another commonly used technique for augmenting the upper jaw when the sinus floor is too close to the proposed implant site. These procedures are part of normal implant planning and are selected when they increase the likelihood of long-term success and stability.
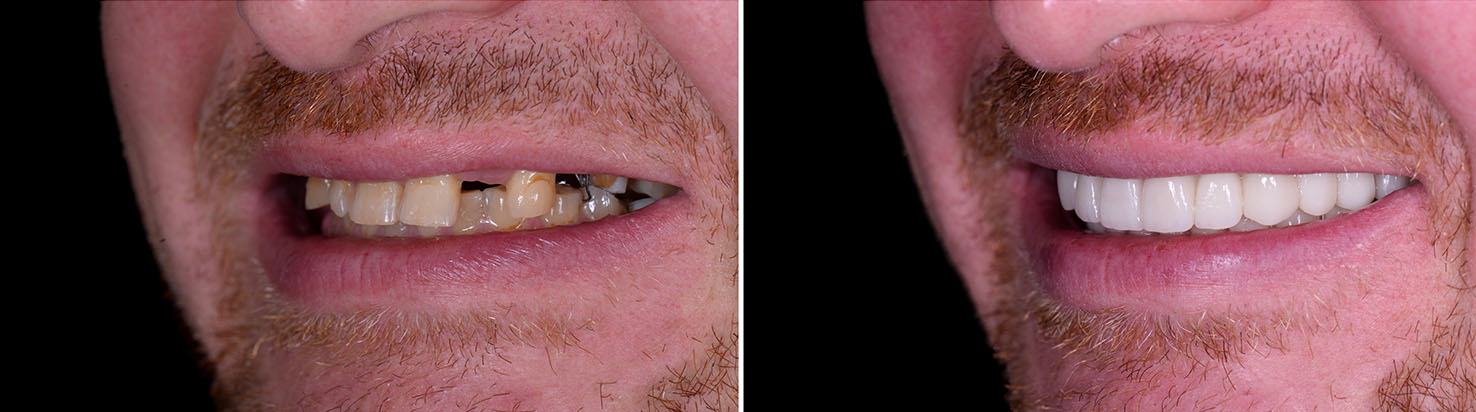
Placing an implant is typically performed as an outpatient procedure. The implant post is positioned precisely in the jawbone, and a brief healing period follows while the implant fuses with the bone — a process known as osseointegration. Healing times vary depending on the site and whether bone augmentation was required, but the goal is always a stable, well-integrated foundation for the final restoration.
We discuss anesthesia and comfort measures beforehand, provide clear aftercare instructions, and schedule follow-up visits to monitor healing. Many patients experience only mild discomfort after surgery, and most return to routine activities within a few days.
Once integration is confirmed, we design the permanent crown, bridge, or denture to match occlusion, function, and aesthetics. Modern restorative materials and techniques allow us to create prostheses that blend naturally with existing teeth while delivering the strength needed for everyday use. The restoration is carefully adjusted to ensure a comfortable bite and a pleasing appearance.
In some cases, immediate restorations can be placed to provide temporary aesthetics and function during healing, with a final, definitive prosthesis fitted once the implant is fully integrated.
Implants require the same attention as natural teeth: brushing, flossing or interdental cleaning, and routine dental checkups. Professional cleanings and periodic exams allow your dental team to monitor the health of the surrounding gum tissue and bone and to address any concerns early. With consistent care, implants can provide many years of dependable service.
We review personalized maintenance plans so patients understand the best cleaning tools and techniques for their specific restorations, whether it’s a single crown or a full-arch prosthesis.
While no dental procedure carries absolute guarantees, implants have a strong track record when placed on healthy foundations and maintained properly. Factors such as oral hygiene, routine professional care, and controlling periodontal disease play a major role in long-term success. Our team focuses on predictable outcomes by combining technology, careful planning, and clear guidance for aftercare.
Choosing implant therapy is an investment in oral health and quality of life — one that many patients find transformative in terms of comfort, function, and confidence.
Dental implants offer a versatile and durable way to replace missing teeth while preserving bone and restoring natural-looking function. From single-tooth crowns to full-arch restorations, implant dentistry can be tailored to meet a wide range of clinical needs and aesthetic goals. With thorough evaluation, precise planning, and attentive follow-up care, implants are a powerful tool for rebuilding healthy, long-lasting smiles.
If you’d like to learn more about implant dentistry or explore whether implants are the right solution for your smile, please contact us for more information.
Dental implants are medical-grade posts that are surgically placed into the jawbone to replace missing tooth roots. Over time the implant integrates with bone in a process called osseointegration, creating a stable foundation for a restoration. A custom crown, bridge, or denture is attached to the implant to replace the visible portion of the tooth and restore chewing and speech function.
Because implants are anchored in bone they transmit normal chewing forces and help preserve bone volume and facial contours. This stability reduces the bone loss that commonly follows untreated tooth loss and supports long-term oral health. When planned and placed correctly, implants provide a predictable, natural-feeling solution for single-tooth and full-arch replacements.
Most adults in generally good health who have adequate bone volume and controlled medical conditions can be considered for implants. We evaluate your overall medical history, current medications, gum health, and habits such as smoking to determine suitability and risk. Many concerns can be managed or treated so that implant therapy becomes a predictable option for a wide range of patients.
Candidacy is determined through a combination of clinical examination and diagnostic imaging rather than a single rule. When preparatory treatments like extractions, periodontal therapy, or bone grafting are needed, these are coordinated to create a healthy foundation for implant placement. Your individualized plan will balance functional needs, aesthetic goals, and long-term stability.
Implant restorations include single crowns, implant-supported bridges, implant-retained overdentures, and full-arch fixed or removable prostheses. Single-tooth implants replace one tooth without altering adjacent teeth, preserving natural structure and function. Bridges and multi-unit restorations use implants to support several connected crowns when multiple neighboring teeth are missing.
For patients missing an entire upper or lower arch, fixed full-arch bridges or removable hybrid dentures can restore a stable, functional set of teeth anchored by a limited number of implants. Implant-retained overdentures clip onto implants to improve retention while remaining removable for cleaning. The choice between fixed and removable designs depends on oral anatomy, hygiene preferences, and functional goals.
Materials and design are selected to match occlusion and aesthetics so restorations blend with existing teeth. In some cases immediate provisional teeth are placed to maintain appearance and function during healing. Final prostheses are fabricated once integration and soft tissue health are confirmed.
The process begins with a detailed consultation that includes a clinical exam, digital X-rays or scans, and a review of your medical and dental history. We discuss restorative options, the number and location of implants needed, and any preparatory procedures required to optimize outcomes. This planning phase establishes a clear sequence of care and sets expectations for timing and recovery.
Surgical placement is typically an outpatient procedure performed with local anesthesia and, when appropriate, sedation for comfort. After the post is placed a healing period allows osseointegration; follow-up visits monitor progress and address any concerns. Once integration is confirmed, impressions or digital records are taken and the final crown, bridge, or denture is fabricated and adjusted for comfort and function.
Healing times vary depending on the implant site, bone quality, and whether grafting was required, but osseointegration commonly takes several months. Many patients experience mild post-operative discomfort for a few days and return to normal activities shortly after surgery. Regular follow-up appointments help ensure healing is progressing as planned and that surrounding tissues remain healthy.
When placed on a healthy foundation and maintained with good oral hygiene, implants have a strong long-term success record. Longevity depends on factors such as placement precision, control of periodontal disease, tobacco use, and routine professional care. With consistent maintenance implants can provide many years of reliable function.
Bone loss at an implant site is a common result of long-standing tooth loss or other local conditions, and grafting rebuilds the foundation to provide adequate support. Bone grafting can be performed at the time of extraction or as a separate preparatory step depending on the clinical situation. The chosen graft material and technique are selected to encourage new bone growth and support predictable implant placement.
Sinus augmentation is a specific grafting technique used in the upper jaw when the sinus floor is too close to the intended implant position. Both procedures are routine in implant dentistry and are recommended only when they increase the likelihood of long-term success. Your treatment plan will clearly explain timing, risks, and expected outcomes so you understand how these steps fit into the overall sequence of care.
Implant placement is usually performed in the dental office with local anesthesia and optional sedation to keep you comfortable. The procedure involves precise positioning of the implant post in the jawbone followed by suturing and specific post-operative instructions. Most patients report only mild swelling or discomfort that can be managed with prescribed or over-the-counter measures and short periods of rest.
Follow-up visits monitor healing and address any early complications promptly to support successful integration. Good oral hygiene, avoiding tobacco, and following dietary recommendations during healing all contribute to a smoother recovery. Your care team will provide detailed pre-op and post-op instructions and remain available for questions throughout the process.
Daily care for implants mirrors care for natural teeth: brush twice daily, clean between teeth and implants with floss or interdental tools, and avoid habits that place excessive force on restorations. Routine professional cleanings and exams allow the dental team to evaluate gum tissue and bone health around implants and to remove any plaque or calculus that accumulates. Personalized hygiene recommendations, including specific tools and techniques, will be provided based on the type of restoration you have.
Controlling periodontal inflammation is essential because surrounding gum disease can compromise implant stability over time. Regular maintenance visits also let us check occlusion and the integrity of crowns, bridges, or denture attachments and make adjustments as needed. With consistent home care and professional oversight implants can remain a dependable part of your oral health plan.
Dental implants are a well-established treatment with predictable outcomes when placed after thorough evaluation and planning. As with any surgical procedure there are potential risks such as infection, nerve irritation, sinus complications, or failure to integrate, and these are minimized through careful technique and follow-up care. Your provider will explain the specific risks that pertain to your case and how they are managed.
Certain medical conditions, medications, or lifestyle factors can increase risk and affect planning; full disclosure of your medical history helps the team tailor treatment and reduce complications. When complications occur early recognition and timely intervention improve the likelihood of a favorable resolution. Emphasizing communication, imaging, and appropriate pre-treatment care supports safety and long-term success.
To explore whether implants are right for you, contact the office to arrange a consultation where diagnostic imaging and a clinical exam can establish candidacy and a treatment roadmap. The team will review your medical and dental history, answer questions about the process, and outline any preparatory steps that may be needed. Clear communication about expectations and next steps helps patients feel informed and comfortable with their plan.
At the office of Brittney K. Craig, DMD our staff coordinates care efficiently and provides detailed pre-op and post-op instructions to support smooth treatment and recovery. We encourage prospective patients to bring a list of questions and to share relevant medical information so the consultation is as productive as possible. If additional specialists or preparatory procedures are required, we will outline how coordination will occur to keep your care organized.